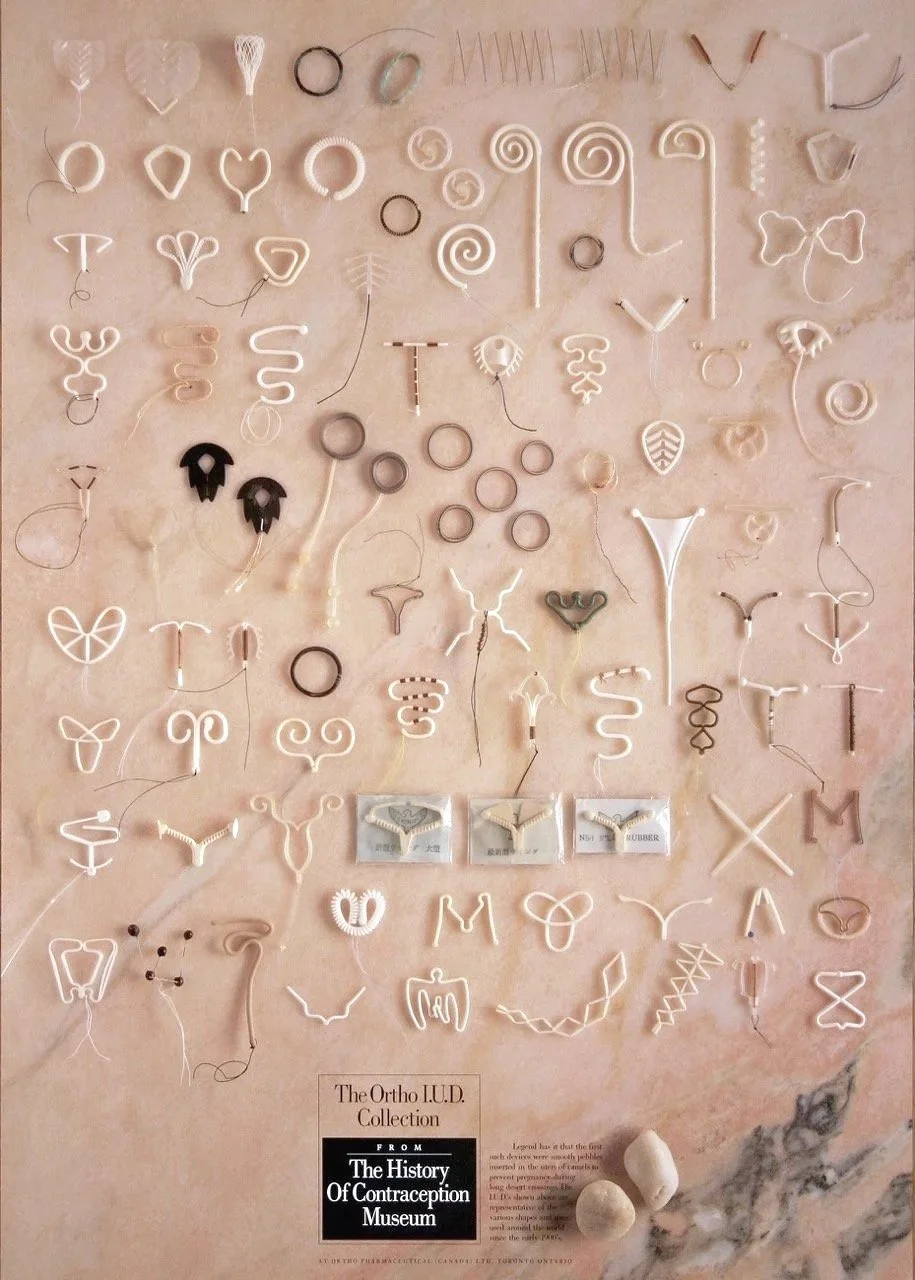The copper IUD
Carolyn Herrera-Perez
Poster, The Ortho i.u.d. Collection. Dittrick Medical History Center, Case Western Reserve University. 20004.020-PosterD.
It’s a little T-shaped plastic device, with copper collars and wire wrapping around its frame. That added metal may look like an element for electric conduction, but actually it makes the object of the most potent contraceptive devices ever developed. Medically known as the CuT380A, this intrauterine device (IUD) has been marketed as the Paragard in the United States since its release in 1988. The official name derives from the element (Cu), its overall shape (resembling a letter “T”), and the total area of the device’s exposed copper surface (380 square millimeters). Many people with uteruses choose the Paragard for its unique qualities: it is immediately effective upon insertion, lasts as long as ten years, and is entirely hormone-free. Unlike IUDs that use hormones, the CuT380A’s active component is the copper itself, which makes it up to 99% effective at preventing pregnancy.
For over a century, IUD design haphazardly followed the arc of prevailing material science. In 1909, the first IUD was made of dried silkworm gut, wound into a ring shape. The silk ring caused a reaction that could prevent pregnancy: when any foreign object is inserted into the uterus, the local area counters by causing inflammation. This response makes the uterine environment hostile to sperm and more difficult for an embryo to implant itself in the uterus lining. All IUDs, then and now, create these effects, but local inflammatory reactions alone are not reliable in preventing pregnancy.
In the 1960s, a significant boom in birth control technology brought “the pill” and second-generation IUDs to the market. True to the spirit of the ‘60s, these devices were often made of innovative, flexible plastics in an array of shapes and sizes: rings, spirals, loops, bowties, triangles, and much more. The new plastics allowed for bulkier forms that were designed to fill the uterine cavity, bringing a lower pregnancy rate and many unwanted side effects like cramping, heavy bleeding, and abdominal pain. Like the silk design from 1909, these IUDs had no “active ingredient,” and because they were considered drug-free the plastic IUDs of the 60s and early 70s did not go through extensive testing by the US Food and Drug Administration (FDA).
One of these second-generation devices came to negatively impact perceptions of IUDs for decades. Introduced in 1971, the Dalkon Shield was fraught with flaws, beginning with its basic design. The crab-shaped plastic device was challenging to insert; worse, the string used to extract it from the uterus was porous, with multiple strands. Like a wick, it pulled bacteria from the vaginal canal into its user’s uterus, which could lead to inflammatory disease, septic infections, miscarriage, and sterilizing injuries. Fifteen women died using the Dalkon Shield, and over 300,000 lawsuits were filed against its makers, the A.H. Robins company. The company sold discounted shields to developing countries even after the FDA took it off the U.S. market in 1974. As a result of the incident, IUD design is now highly regulated by the FDA. Still, overall IUD usage dropped dramatically, and to this day the use of this technology in the United States lags that of other countries.
While the Dalkon tragedy unfolded, new scientific research suggested the positive effect of copper for contraception. To better fit the contours of the uterus, American doctor Howard Tatum made a device in the form of a plastic T. At the same time, Jaimie Zipper, a doctor in Chile, discovered that placing a copper wire in one horn of a rabbit’s uterus prevented that portion from pregnancy. Tatum’s T-shaped design still had a pregnancy rate of 18%. But when copper was added, the combination produced a remarkable effect: “a pregnancy rate of just 1 percent after a twelve-month trial ending in 1970.” A year later, the FDA reclassified copper IUDs as a drug, warranting extensive testing before the CuT200’s release in 1976. In 1984 an updated version with more copper –the CuT380A– was approved and brand-named the Paragard for the U.S. market. Still available today, its introduction gradually changed opinion regarding the technology, making way for the hormone-releasing IUDs of the 2000s.
Curiously, there is no widespread agreement on why the metal works in copper-bearing devices. Through a simple but notoriously painful insertion process, the IUD is placed in the uterus. Copper ions make the area spermicidal by impacting sperm motility, or “movability.” When the United Nations studied the first Copper T, the CuT200, they offered a surprising explanation—the detachment of sperm heads from their tails. In other words, the metal is toxic to sperm but it remains unclear exactly why this is the case. Over time, as the metal slowly dissolves, the device gradually becomes less effective. Unique to copper contraceptives, typical side effects include mild to unbearable cramping and a heavier, more painful menstrual period.
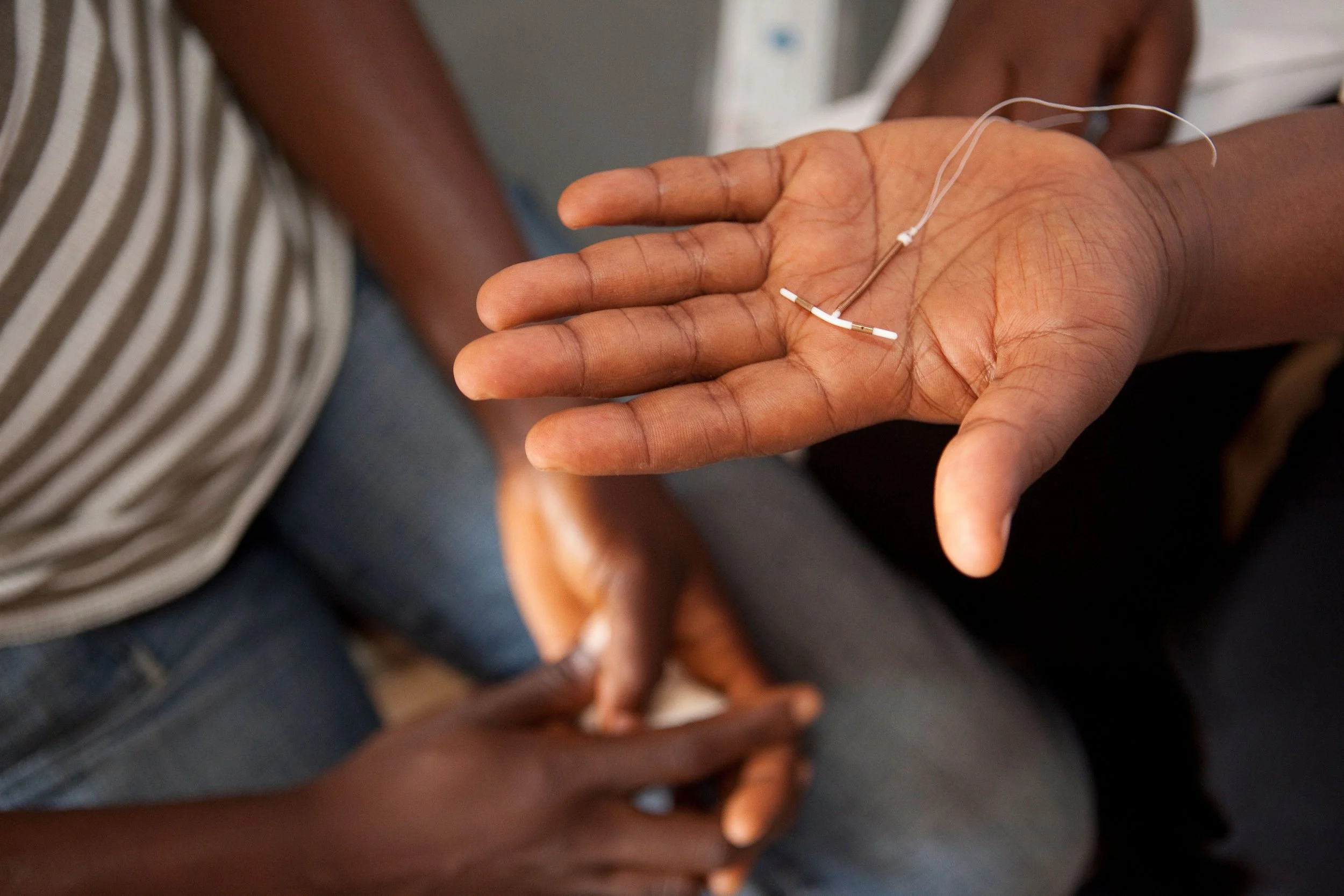
A midwife talks about an intrauterine device with a patient at a reproductive health clinic in Yaounde, Cameroon, West Africa. Jake Lyell, Alamy Stock Photo.